Geriatric Cardiology Details
Geriatric Cardiology. Mobile Phone 01797522136. Geriatric Cardiology is a branch of cardiology discusses with the geriatric common cardiovascular diseases. These diseases are congestive heart failure, coronary artery disease, cardiac valvular disease, and arrhythmias in elderly patients.
Geriatric Cardiology is an important subject for all cardiology students. This subject is studied in some course of HRTD Medical Institute. The courses are PDT Cardiology, PDT Medicine, Caregiving Long Course, etc.
Congestive Heart Failure
If the heart cannot pump the amount of blood that the body needs every minute, it is called heart failure. Heart failure in which fluid accumulates in various tissues is called congestive heart failure. Congestive heart failure usually causes fluid to accumulate in the lungs and legs.
প্রতি মিনিটে দেহে যে পরিমাণ রক্ত সরবরাহ দরকার হার্ট যদি সেই পরিমাণ রক্ত সরবরাহ না করতে পারে তবে তাকে হার্ট ফেইলর বলে । যে হার্ট ফেইলরে বিভিন্ন টিসুতে তরল পদার্থ জমে যায় তাকে কনজেস্টিভ হার্ট ফেইলর বলে । কনজেস্টিভ হার্ট ফেইলে সাধারনত ফুসফুস এবং পায়ে তরল জমা হয় ।
Types of congestive heart failure
Types of congestive heart failure include:
- Left-sided heart failure.
- Right-sided heart failure.
- High-output heart failure. This is a rare type of congestive heart failure.
How common is congestive heart failure?
More than 6 million people in the United States have congestive heart failure. It’s the leading cause of hospitalization in people older than 65.
Symptoms and Causes of congestive heart failure
What are the congestive heart failure symptoms?
Congestive heart failure symptoms include:
- Shortness of breath.
- Waking up short of breath at night.
- Chest pain.
- Heart palpitations.
- Fatigue when you’re active.
- Swelling in your ankles, legs and abdomen.
- Weight gain.
- Need to urinate while resting at night.
- A dry, hacking cough.
- A full (bloated) or hard stomach.
- Loss of appetite or upset stomach (nausea).
Sometimes, you may have mild symptoms of congestive heart failure or none at all. This doesn’t mean you don’t have heart failure anymore. Symptoms of heart failure can range from mild to severe and may come and go.
Unfortunately, congestive heart failure usually gets worse over time. As it worsens, you may have more or different signs or symptoms.
What causes congestive heart failure?
Causes of congestive heart failure include:
- Coronary artery disease and/or heart attack.
- Cardiomyopathy (genetic or viral).
- Heart issues present at birth (congenital heart disease).
- Diabetes.
- High blood pressure (hypertension).
- Arrhythmia.
- Kidney disease.
- A body mass index (BMI) higher than 30.
- Tobacco and recreational drug use.
- Alcohol use.
- Medications such as cancer drugs (chemotherapy).
Left-sided heart failure is the most common cause of right-sided heart failure. When your left ventricle isn’t working correctly, it allows blood to back up. At some point, this backup affects your right ventricle. Other causes include certain lung problems and issues in other organs.
What are the risk factors for congestive heart failure?
Risk factors for congestive heart failure include:
- Being older than 65.
- Using tobacco products, cocaine or alcohol.
- Having an inactive (sedentary) lifestyle.
- Eating foods that have a lot of salt and fat.
- Having high blood pressure.
- Having coronary artery disease.
- Having a heart attack.
- Having a family history of congestive heart failure.
What are the complications of congestive heart failure?
Some of the complications from congestive heart failure include:
- Irregular heartbeat.
- Sudden cardiac arrest.
- Heart valve problems.
- A collection of fluid in your lungs.
- Pulmonary hypertension.
- Kidney damage.
- Liver damage.
- Malnutrition.
Diagnosis and Tests congestive heart failure
How is congestive heart failure diagnosed?
Your healthcare provider will ask you about your symptoms and medical history. They may ask you about:
- Other health conditions you have.
- A family history of heart disease or sudden death.
- Your use of tobacco products.
- How much alcohol you drink.
- Any history of chemotherapy and/or radiation.
- The medications you take.
You’ll also have a physical exam. Your provider will look for signs of congestive heart failure and diseases that may have made your heart muscle weak or stiff.
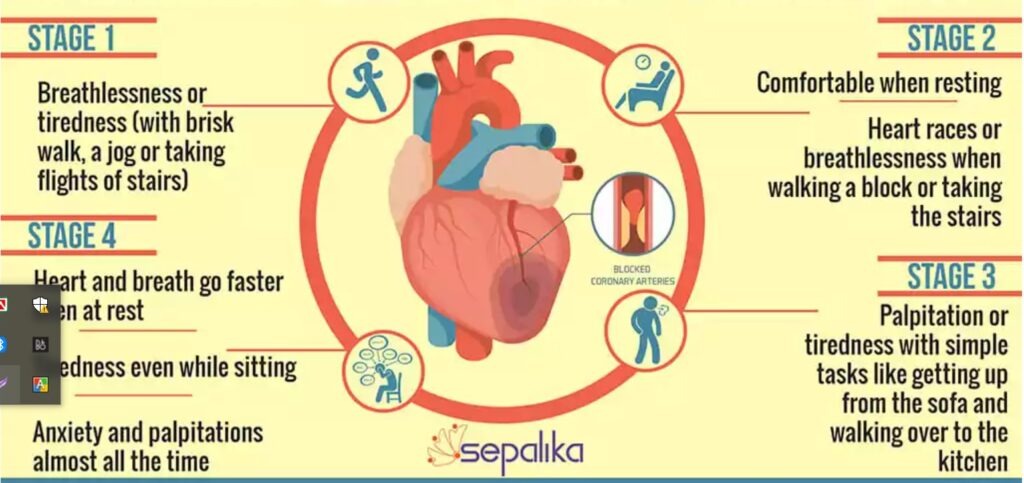
What are the four stages of congestive heart failure?
Heart failure is a chronic condition that gets worse with time. There are four heart failure stages (Stages A, B, C and D). They range from having a high risk of developing heart failure to having advanced heart failure.
Stage A
Stage A (pre-heart failure) means you’re at a high risk of developing heart failure because you have a family history of congestive heart failure or you have one or more of these medical conditions:
- Hypertension.
- Diabetes.
- Coronary artery disease.
- Metabolic syndrome.
- History of alcohol use disorder.
- History of rheumatic fever.
- Family history of cardiomyopathy.
- History of taking drugs that can damage your heart muscle, such as some cancer drugs.
Stage B
Stage B (pre-heart failure) means your left ventricle isn’t working well and/or is structurally abnormal but you’ve never had symptoms of heart failure.
Stage C
People with Stage C heart failure have a congestive heart failure diagnosis and currently have or previously had signs and symptoms of the condition.
Stage D and reduced EF (ejection fraction)
People who have Stage D HFrEF (heart failure with reduced ejection fraction) have advanced symptoms that don’t get better with treatment. This is the final stage of heart failure.
What tests will be done to diagnose congestive heart failure?
Common tests to identify congestive heart failure, its stage and its cause include:
- Blood tests.
- Cardiac catheterization.
- Chest X-ray.
- Echocardiogram.
- Heart MRI (magnetic resonance imaging).
- Cardiac computed tomography (CT).
- Electrocardiogram (EKG or ECG).
- Multigated Acquisition Scan (MUGA scan).
- Stress test.
- Genetic testing.
Management and Treatment of congestive heart failure
How is congestive heart failure treated?
Your treatment will depend on the type of heart failure you have and, in part, what caused it. Medications and lifestyle changes are part of every heart failure treatment plan. Your healthcare provider will talk to you about the best treatment plan for you.
There’s no cure for heart failure. As congestive heart failure gets worse, your heart muscle pumps less blood to your organs, and you move toward the next stage of heart failure. Since you can’t move backward through the heart failure stages, the goal of treatment is to keep you from moving forward through the stages or to slow down the progression of your heart failure.
Stage A treatment
Treatment for people with Stage A heart failure includes:
- Regular exercise, such as walking every day.
- No tobacco products.
- Treatment for high blood pressure (medication, low-sodium diet, active lifestyle).
- Treatment for high cholesterol.
- No alcohol or recreational drugs.
- Angiotensin-converting enzyme inhibitor (ACE-I) or an angiotensin II receptor blocker (ARB) if you have coronary artery disease, diabetes, high blood pressure or other vascular or cardiac conditions.
Stage B treatment
Treatment for people with Stage B heart failure includes:
- Treatments for Stage A.
- Angiotensin-converting enzyme inhibitor (ACE-I) or angiotensin II receptor blocker (ARB) if your EF is 40% or lower.
- Beta-blocker if you’ve had a heart attack and your EF is 40% or lower (if you aren’t already taking one).
- Aldosterone antagonist if you’ve had a heart attack or if you have an EF of 35% or less.
- Possible surgery or intervention as a treatment for coronary artery blockage, heart attack, valve disease (valve repair or replacement) or congenital heart disease.
Stage C treatment
Treatment for people with Stage C HFrEF includes:
- Treatments from Stages A and B.
- Beta-blocker.
- Aldosterone antagonist.
- Sodium-glucose transport 2 inhibitors (SGLT2i).
- Hydralazine/nitrate combination if other treatments don’t stop your symptoms and you’re African American.
- Medications that slow your heart rate if your heart rate is faster than 70 beats per minute and you still have symptoms.
- A diuretic (“water pill”) if symptoms continue.
- Restriction of sodium (salt) in your diet.
- Weight tracking every day. Tell your healthcare provider if you gain or lose more than 4 pounds.
- Possible fluid restriction.
- Possible cardiac resynchronization therapy (biventricular pacemaker).
- Possible implantable cardiac defibrillator (ICD) therapy.
If the treatment improves or stops your symptoms, you still need to continue treatment to slow the progression to Stage D.
Stage D treatment
Treatment for people who have Stage D heart failure includes treatments for Stages A, B and C. In addition, it includes evaluation for more advanced treatment options, including:
- Heart transplant.
- Ventricular assist devices.
- Heart surgery.
- Continuous infusion of inotropic drugs.
- Palliative or hospice care.
Stages C and D with preserved EF
Treatment for people with Stage C and Stage D heart failure and preserved EF (HFpEF) includes:
- Treatments for Stages A and B.
- Medications for the treatment of medical conditions that can cause heart failure or make it worse, such as atrial fibrillation, high blood pressure, diabetes, obesity, coronary artery disease, chronic lung disease, high cholesterol and kidney disease.
- Diuretic (“water pill”) to reduce or relieve symptoms.
It’s very important for you to manage your other health conditions, such as:
- Diabetes.
- Kidney disease.
- Anemia.
- High blood pressure.
- Thyroid disease.
- Asthma.
- Chronic lung disease.
Some conditions have signs and symptoms similar to congestive heart failure. If you have new or worsening nonurgent symptoms, tell your healthcare provider.
Complications/side effects of the treatment
Complications of congestive heart failure treatments may include:
- Hypotension.
- Kidney failure.
- Infections from frequent hospital visits that involve central IVs.
Prevention of congestive heart failure
How can I lower my risk of congestive heart failure?
Although you can’t change some risk factors like age, family history or race, you can change your lifestyle to give yourself the best chance of preventing heart failure. Things you can do include:
- Staying at a weight that’s healthy for you.
- Eating foods that are good for your heart.
- Exercising regularly.
- Managing your stress.
- Stopping the use of tobacco products.
- Not drinking alcohol.
- Not using recreational drugs.
- Taking care of other medical conditions you have that can increase your risk.
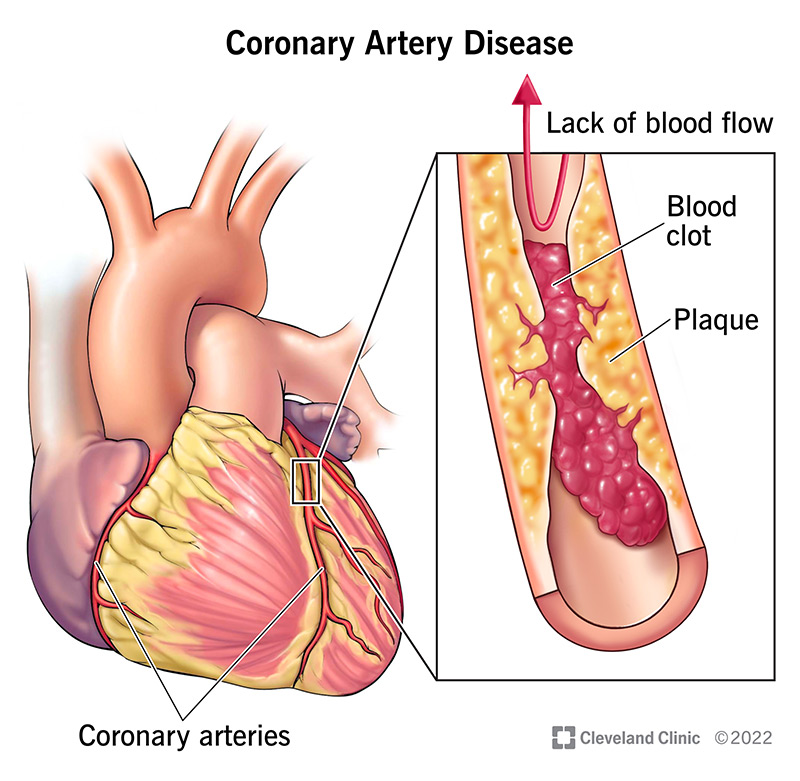
What is coronary artery disease?
Coronary artery disease (CAD) is a narrowing or blockage of your coronary arteries, which supply oxygen-rich blood to your heart. This happens because, over time, plaque (including cholesterol) buildup in these arteries limits how much blood can reach your heart muscle.
Picture two traffic lanes that merge into one due to construction. Traffic keeps flowing, just more slowly. With CAD, you might not notice anything is wrong until the plaque triggers a blood clot. The blood clot is like a concrete barrier in the middle of the road. Traffic stops. Similarly, blood can’t reach your heart, and this causes a heart attack.
You might have CAD for many years and not have any symptoms until you experience a heart attack. That’s why CAD is a “silent killer.”
Other names for CAD include coronary heart disease (CHD) and ischemic heart disease. It’s also what most people mean when they use the general term “heart disease.”
Coronary artery disease types
There are two main forms of coronary artery disease:
- Stable ischemic heart disease: This is the chronic form. Your coronary arteries gradually narrow over many years. Over time, your heart receives less oxygen-rich blood. You may feel some symptoms, but you’re able to live with the condition day to day.
- Acute coronary syndrome: This is the sudden form that’s a medical emergency. The plaque in your coronary artery suddenly ruptures and forms a blood clot that blocks blood flow to your heart. This abrupt blockage causes a heart attack.
How common is coronary artery disease?
Coronary artery disease is very common. Over 18 million adults in the U.S. have coronary artery disease. That’s roughly the combined populations of New York City, Los Angeles, Chicago and Houston.
In 2021, coronary artery disease killed 375,500 people in the U.S.
Coronary artery disease is the leading cause of death in the U.S. and around the world.
Symptoms and Causes
What are the symptoms?
You may have no symptoms of coronary artery disease for a long time. Plaque buildup takes many years, even decades. But as your arteries narrow, you may notice mild symptoms. These symptoms mean your heart is pumping harder to deliver oxygen-rich blood to your body.
Symptoms of chronic CAD include:
- Stable angina: This is the most common symptom. Stable angina is temporary chest pain or discomfort that comes and goes in a predictable pattern. You’ll usually notice it during physical activity or emotional distress. It goes away when you rest or take nitroglycerin (medicine that treats angina).
- Shortness of breath (dyspnea): Some people feel short of breath during light physical activity.
Sometimes, the first coronary artery disease symptom is a heart attack.
What causes coronary artery disease?
Atherosclerosis causes coronary artery disease. Atherosclerosis is the gradual buildup of plaque in arteries throughout your body. When the plaque affects blood flow in your coronary arteries, you have coronary artery disease.
Plaque consists of cholesterol, waste products, calcium and fibrin (a substance that helps your blood clot). As plaque collects along your artery walls, your arteries become narrow and stiff.
Plaque can clog or damage your arteries, which limits or stops blood flow to a certain part of your body. When plaque builds up in your coronary arteries, your heart muscle can’t receive enough blood. So, your heart can’t get the oxygen and nutrients it needs to work properly (myocardial ischemia). It leads to chest discomfort (angina) and puts you at risk of a heart attack.
People who have plaque buildup in their coronary arteries often have buildup elsewhere in their body, too. This can lead to conditions like carotid artery disease and peripheral artery disease (PAD).
Is it genetic?
Partly. Family history affects your risk of coronary artery disease, but many other risk factors have nothing to do with your genetics. The choices you make every day add up to a big impact on your risk of CAD.
What are the risk factors for coronary artery disease?
There are many risk factors for coronary artery disease. You can’t change all of them, but you can manage some of them by making lifestyle changes or taking medications. Talk with your provider about what you can do about these risk factors:
- Being older than 45 if you’re male or over 55 if you’re female.
- Having a biological family member with heart disease, especially a father or brother with a diagnosis before age 55 or mother or sister before age 65.
- Eating a lot of saturated fat or refined carbohydrates.
- Not exercising enough.
- Not getting enough sleep.
- Smoking, vaping or other tobacco use.
- Having atherosclerosis.
- High blood pressure.
- High LDL (“bad”) cholesterol.
- Low HDL (“good”) cholesterol.
- High triglycerides (hypertriglyceridemia).
- Anemia.
- Autoimmune diseases, including lupus and rheumatoid arthritis.
- Chronic kidney disease.
- Diabetes.
- HIV/AIDS.
- Metabolic syndrome.
- A body mass index (BMI) higher than 25.
- Sleep disorders like sleep apnea.
- Early menopause (before age 40).
- Endometriosis.
- History of gestational diabetes, eclampsia or preeclampsia.
- Use of hormonal birth control.
What are the complications of coronary artery disease?
The main complication of coronary artery disease is a heart attack. This is a medical emergency that can be fatal. Your heart muscle starts to die because it’s not receiving enough blood. You need prompt medical attention to restore blood flow to your heart and save your life.
Over the years, CAD can also weaken your heart and lead to complications, including:
- Arrhythmias (abnormal heart rhythms like atrial fibrillation).
- Cardiac arrest.
- Cardiogenic shock.
- Heart failure.
Diagnosis and Tests
How is coronary artery disease diagnosed?
Healthcare providers diagnose coronary artery disease through a physical exam and testing.
During your physical exam, your provider will:
- Measure your blood pressure.
- Listen to your heart with a stethoscope.
- Ask what symptoms you’re experiencing and how long you’ve had them.
- Ask you about your medical history.
- Ask you about your lifestyle.
- Ask you about your family history. They’ll want to know about heart disease among your biological parents and siblings.
All of this information will help your provider determine your risk for heart disease.
What tests will be done?
Your provider may also recommend one or more tests to assess your heart function and diagnose CAD. These include:
- Blood tests.
- Cardiac catheterization.
- Computed tomography (CT) coronary angiogram.
- Heart MRI (magnetic resonance imaging).
- Coronary calcium scan.
- Echocardiogram (echo).
- Electrocardiogram (EKG/ECG).
- Exercise stress test.
- Chest X-ray.
Management and Treatment
How is coronary artery disease treated?
Coronary artery disease treatment often includes lifestyle changes, risk factor management and medications. Some people may also need a procedure or surgery.
Your healthcare provider will talk with you about the best treatment plan for you. It’s important to follow your treatment plan so you can lower your risk of serious complications from CAD.
Lifestyle changes
Lifestyle changes play a big role in treating coronary artery disease. Such changes include:
- Don’t smoke, vape or use any tobacco products.
- Eat heart-healthy foods low in sodium, saturated fat, trans fat and sugar. The Mediterranean diet is a proven way to lower your risk of a heart attack or stroke.
- Exercise: Aim for 30 minutes of walking (or other activities) five days a week.
- Limit alcohol.
Be sure to talk with your provider before starting any new exercise program. Your provider can also offer guidance on lifestyle changes tailored to your needs. They may recommend smoking cessation options or meeting with a dietitian to discuss healthy eating plans.
Risk factor management
Managing your risk factors for CAD can help slow down the progression of your disease. Work with your provider to manage the following conditions:
- Diabetes.
- High blood pressure.
- High cholesterol.
- High triglycerides (hypertriglyceridemia).
- Having a BMI higher than 25.
Medications
Medications can help you manage your risk factors and treat symptoms of coronary artery disease. Your provider may prescribe one or more medications that:
- Lower your blood pressure.
- Lower your cholesterol.
- Manage stable angina, like nitroglycerin and ranolazine.
- Reduce your risk of blood clots.
Procedures and surgeries
Some people need a procedure or surgery to manage coronary artery disease, including:
- Percutaneous coronary intervention (PCI): This minimally invasive procedure has another name — coronary angioplasty. Your provider reopens your blocked artery to help blood flow through it better. They may also insert a stent to help your artery stay open.
- Coronary artery bypass grafting (CABG): This surgery creates a new path for your blood to flow around blockages. This “detour” restores blood flow to your heart. CABG helps people who have severe blockages in several coronary arteries.
Complications/side effects of the treatment
Complications or side effects of coronary artery disease treatments may include:
- Bleeding.
- Diarrhea.
- Dizziness.
- Cough.
- Blood clot.
- Coronary artery puncture.
- Infection.
- Abnormal heart rhythms.
- Cardiac tamponade.
How long does it take to recover from this treatment?
After PCI (angioplasty), you can usually get back to normal activities within a week. After CABG (bypass surgery), you’ll be in the hospital for more than a week. After that, it’ll take six to 12 weeks for a full recovery.
Prevention
Can coronary artery disease be prevented?
You can’t always prevent coronary artery disease because some risk factors are out of your control. But you can lower your risk of coronary artery disease and help prevent it from getting worse in these ways:
- Commit to quitting smoking and all tobacco use.
- Eat heart-healthy foods.
- Get enough sleep.
- Stay at a weight that’s healthy for you.
- Learn your risk for heart disease.
- Limit alcohol use.
- Move around more.
- Keep taking your medications.
What is heart valve disease?
Heart valve disease refers to any of several conditions that prevent one or more of the valves in your heart from working right. Left untreated, heart valve disease may reduce blood flow and cause your heart to work harder. Untreated heart valve disease can become life-threatening.
But there’s hope. In many cases, your healthcare provider can do surgery or a minimally invasive procedure to repair or replace your heart valves. This restores normal function and allows you to return to normal activities.
The four valves in your heart make sure blood flows in only one direction through your heart. Your valves consist of small flaps of tissue (called leaflets) that open to allow blood to move forward through your heart during half of your heartbeat. These leaflets close to prevent blood from flowing backward during the other half of your heartbeat.
Your heart’s valves are:
- Mitral (between your left atrium and left ventricle)
- Tricuspid (between your right atrium and right ventricle)
- Aortic (between your left ventricle and aorta)
- Pulmonary (between your right ventricle and pulmonary artery)

Types of heart valve disease
There are different types of heart valve disease: stenosis, regurgitation, prolapse and atresia. They can affect more than one valve.
Stenosis
Tissues forming the valve leaflets become stiffer, narrowing your valve opening and reducing the amount of blood that can flow through it. Mild narrowing may not reduce the overall functioning of your heart. But the valve can become so narrow (stenotic) that it reduces your heart’s function, makes your heart pump harder and puts it under strain. As a result, the rest of your body may not get enough blood flow.
Regurgitation
Also known as insufficiency or “leaky valve,” this happens when your leaflets don’t close completely. This lets blood leak backward across your valve. Your heart has to pump harder to make up for this backward flow, and the rest of your body may get less blood flow.
Prolapse
Your mitral valve may not close tightly because the leaflets are extra stretchy. They go back into your left atrium when your heart beats. This is usually harmless, but can lead to regurgitation in some people.
Atresia
Valvular atresia happens when a heart valve forms without an opening before birth. Healthcare providers usually diagnose this very early in infancy.
How common is heart valve disease?
About 2.5% of Americans — many of them older adults — have heart valve disease. Each year, roughly 27,000 people die from heart valve disease in the United States. Mitral valve prolapse is a common heart valve problem.
Symptoms and Causes
What are the first signs of heart valve problems?
Many people with heart valve disease don’t have symptoms. But when the condition worsens over time, your heart beats harder to make up for the reduced blood flow.
Heart valve disease symptoms may include:
- Fatigue (This may be your first symptom.)
- Increasing shortness of breath, especially with physical activity
- Palpitations (skipped beats or a flip-flop feeling in your chest)
- Edema (swelling of your ankles, feet or abdomen)
- Weakness or dizziness
- Quick weight gain
- Chest pain, especially when you exert yourself
What causes heart valve disease?
Common heart valve disease causes include:
- Rheumatic fever from strep throat that wasn’t treated
- Heart attack that damages your heart
- High blood pressure (advanced)
- A congenital (present at birth) issue, like a pulmonary or aortic valve that didn’t develop right
- Decline or calcification of the valve tissue, with loss of function over time
- Thoracic aortic aneurysm (widening of your aorta, which stretches the aortic valve leaflets and can cause leakage)
- Heart failure
- Infection in your heart (infective endocarditis)
- Lupus
- Marfan syndrome
Risk factors
Risk factors that give you a greater chance of getting heart valve disease include:
- Using tobacco products
- Eating foods that aren’t nutritious
- Not getting physical activity
- Having certain conditions like diabetes or high blood pressure
- Getting radiation treatment for cancer
- Having a pacemaker or defibrillator (ICD)
- Being male
- Getting older
What are the complications of heart valve disease?
Untreated valve disease may eventually lead to:
- Heart failure
- Abnormal heart rhythms (arrhythmia)
- Blood clots
- High blood pressure in your pulmonary arteries (pulmonary hypertension)
- Stroke
- Cardiac arrest
Diagnosis and Tests
How is heart valve disease diagnosed?
During a physical examination, a healthcare provider may find these signs of heart valve disease:
- Fluid in your lungs
- An enlarged heart
- A heart murmur, which could mean blood is moving through a narrow or leaky valve
- Swelling in your ankles
Several medical tests can also show heart valve disease. Repeating tests over time can help your provider see the progress of your valve disease and make decisions about your treatment. Valve disease can get worse over time. You may hear a provider describe valve disease with a letter for its stage. Stages start with A and end with D, which is the most severe.
What tests will be done?
Tests for heart valve disease diagnosis include:
- Echocardiogram (heart ultrasound) — A moving image of your heart using sound waves from a handheld wand placed on your chest
- Transesophageal echocardiogram (TEE) — An ultrasound of your heart that uses a probe with a transducer down your esophagus, which sits very close to your heart
- Exercise stress echocardiogram — A test that shows how your valves and heart function after you walk on a treadmill or ride a bike.
- Chest X-ray — A quick X-ray scan of your chest.
- Cardiac catheterization (angiogram) — X-ray movies of your coronary arteries, heart chambers and heart valves.
- Electrocardiogram (EKG or ECG) — Small electrode patches attached to your skin record your heart’s electrical activity.
- Magnetic resonance imaging (MRI) — Radio waves and a magnet work together to create high-quality images of your heart.
Management and Treatment
How is heart valve disease treated?
Heart valve disease treatments depend on the cause and may include:
- Protecting your valve from further damage
- Taking medications
- Having surgery or invasive procedures if necessary
- Seeing your cardiologist (heart doctor) for regular visits
Although you can’t undo damage to a heart valve, you can treat the issue. The decision to prescribe medical treatment, surgical repair or surgical replacement depends on several factors, including:
- The type of valve disease
- The severity of the damage
- Your age
- Your medical history
If you’re pregnant and have heart valve disease, you can get extra rest and/or take certain medicines that are safe for your baby.
If you know about your valve disease before pregnancy, ask your healthcare provider if you should have tests or see a cardiologist before trying to become pregnant. This can help ensure that you get the right treatment before and during pregnancy. If you have a severe valve problem, your provider may recommend valve repair or replacement before pregnancy.
Medications
Although medicines can’t cure heart valve disease, they — and a healthy lifestyle — can help with symptoms and decrease your chance of having a stroke or cardiac arrest. You may be able to stop taking some medications after valve surgery, but you may need to take other medicines for the rest of your life.
Your healthcare provider may prescribe medications to help you with:
- Preventing arrhythmias or blood clots
- Bringing down your blood pressure or cholesterol levels
- Treating heart failure or coronary artery disease
Surgical repair or replacement
Heart valve disease is a problem with the opening or closing of your leaflets, and you may need surgery to repair or replace your valve. Some infants who have congenital (present at birth) valve issues need surgery during childhood.
Usually, the surgeon and cardiologist will know which treatment will be best before surgery day. Other times, the surgeon decides during surgery, when they can see your valve.
Often, providers may combine valve surgery with other procedures (like bypass surgery or surgery to treat atrial fibrillation) to fully treat your heart disease.
Heart valve repair allows your surgeon to fix your faulty valve, often without the use of artificial parts. In some cases, like a narrow mitral valve, your provider may use a balloon on a catheter (valvuloplasty) to widen your valve. They may perform an annuloplasty to fix or reinforce the ring around your valve so it closes better.
The advantages of valve repair are:
- Lower risk of infection
- Decreased need for lifelong blood thinner medication
- Preserved heart muscle strength and function
Surgeons have to replace valves they can’t repair. Replacing your heart valve involves removing your old valve and sewing a new valve to the ring-shaped part of your old one. The new valve could be mechanical or biological (made with tissue from a human, cow or pig). These replacement valves can provide function when repair can’t. But depending on the type of valve you get, you may have to take certain medications to prevent blood clots or get a new valve again in 10 or 15 years.
Depending on the type of valve problem and your other medical conditions, you may be able to have minimally invasive valve repair or replacement.
Complications of treatment
Older people and those whose health isn’t good to begin with have a higher risk of complications from valve replacement surgery.
Complications, which are rarely fatal, may include:
- Infection
- Atrial fibrillation or another type of abnormal heart rhythm
- Bleeding
- Blood clots
- Kidney failure
- Stroke or transient ischemic attack (TIA)
How long does it take to recover from heart valve surgery?
You may be in the hospital for about five to seven days after heart valve surgery. After that, it can take about four to eight weeks to recover. Your provider may recommend cardiac rehab, a carefully monitored program to assist with your recovery.
Prevention
How can I reduce my risk of heart valve disease?
Although you can’t change some risk factors, like growing older, there are things you can do that may reduce your risk of heart valve disease. These include:
- Getting treatment quickly for infections
- Being physically active
- Eating heart-healthy foods
- Staying at a weight that’s healthy for you
- Continuing to take medicine for high blood pressure and/or high cholesterol if you have those conditions
- Not using tobacco products
- Not using recreational drugs, especially IV drugs, which increase your risk for heart valve infection
Protecting your valve from further damage
If you have heart valve disease, ask your healthcare provider about the increased risk of getting infective endocarditis. This infection can damage or destroy your heart valves and can be fatal. You’re at risk even if you had surgery to repair or replace your valve. To prevent infective endocarditis:
- Tell your medical and dental providers that you have valve disease
- Call your provider if you have symptoms of an infection
- Take good care of your teeth and gums
- Ask your cardiologist if you should take antibiotics before any dental procedures, major or minor surgeries or invasive tests
Heart Arrhythmia
A heart arrhythmia (uh-RITH-me-uh) is an irregular heartbeat. A heart arrhythmia occurs when the electrical signals that tell the heart to beat don’t work properly. The heart may beat too fast or too slow. Or the pattern of the heartbeat may be inconsistent.
A heart arrhythmia may feel like a fluttering, pounding or racing heartbeat. Some heart arrhythmias are harmless. Others may cause life-threatening symptoms.
There are times when it is OK to have a fast or slow heartbeat. For example, the heart may beat faster with exercise or slow down during sleep.
Heart arrhythmia treatment may include medicines, devices such as pacemakers, or a procedure or surgery. The goals of treatment are to control or get rid of fast, slow or otherwise irregular heartbeats. A heart-healthy lifestyle can help prevent heart damage that can trigger some heart arrhythmias.
Types
In general, heart arrhythmias are grouped by the speed of the heart rate. For example:
- Tachycardia (tak-ih-KAHR-dee-uh) is a fast heartbeat. The heart rate is greater than 100 beats a minute.
- Bradycardia (brad-e-KAHR-dee-uh) is a slow heartbeat. The heart rate is less than 60 beats a minute.
Fast heartbeat, called tachycardia
Types of tachycardias include:
- Atrial fibrillation (AFib). Chaotic heart signaling causes a rapid, uncoordinated heartbeat. AFib may be temporary and start and stop on its own. But some episodes may not stop unless treated. AFib has been linked to stroke.
- Atrial flutter. Atrial flutter is similar to AFib, but the heartbeats are more organized. Atrial flutter also is linked to stroke.
- Supraventricular tachycardia. This broad term includes irregular heartbeats that start above the lower heart chambers, called the ventricles. Supraventricular tachycardia causes episodes of a pounding heartbeat that start and stop suddenly.
- Ventricular fibrillation. Rapid, chaotic electrical signals cause the lower heart chambers to quiver instead of squeezing in a coordinated way. This serious problem can lead to death if a regular heart rhythm isn’t restored within minutes. Most people with ventricular fibrillation have an underlying heart disease or had a serious injury.
- Ventricular tachycardia. This rapid, irregular heart rate starts with faulty electrical signals in the lower heart chambers, called the ventricles. The rapid heart rate doesn’t let the ventricles properly fill with blood. So the heart may not be able to pump enough blood to the body. Ventricular tachycardia may not cause serious problems in people with otherwise healthy hearts. In those with heart disease, ventricular tachycardia can be an emergency that needs immediate medical care.
Slow heartbeat, called bradycardia
A heart rate below 60 beats a minute is considered bradycardia. But a low resting heart rate doesn’t always mean there’s a problem. If you’re physically fit, your heart may be able to pump enough blood to the body with less than 60 beats a minute.
If you have a slow heart rate and your heart isn’t pumping enough blood, you may have a type of bradycardia. Types of bradycardias include:
- Sick sinus syndrome. The sinus node sets the pace of the heart. If the node doesn’t work properly, the heart rate may switch between too slow and too fast. Sick sinus syndrome can be caused by scarring near the sinus node that slows, disrupts or blocks heartbeat signals. The condition is most common among older adults.
- Conduction block. A block of the heart’s electrical pathways can cause the signals that trigger the heartbeats to slow down or stop. Some blocks may cause no symptoms. Others may cause skipped beats or slowed heartbeats.
Premature heartbeats
Premature heartbeats are extra beats that occur one at a time, sometimes in patterns that alternate with a regular heartbeat. If the extra beats come from the top chamber of the heart, they are called premature atrial contractions (PACs). If they come from the bottom chamber, they are called premature ventricular contractions (PVCs).
A premature heartbeat may feel like your heart skipped a beat. These extra beats are generally not a concern. They rarely mean you have a more serious condition. Still, a premature beat can trigger a longer lasting arrhythmia, especially in people with heart disease. Occasionally, having very frequent premature ventricular beats may lead to a weak heart.
Premature heartbeats may occur when resting. Stress, heavy exercise and the use of stimulants, such as caffeine or nicotine, also may cause premature heartbeats.
Symptoms
A heart arrhythmia may not cause any symptoms. The irregular heartbeat may be noticed during a health checkup for another reason.
Symptoms of an arrhythmia may include:
- A fluttering, pounding or racing feeling in the chest.
- A fast heartbeat.
- A slow heartbeat.
- Chest pain.
- Shortness of breath.
Other symptoms may include:
- Anxiety.
- Feeling very tired.
- Lightheadedness or dizziness.
- Sweating.
- Fainting or almost fainting.
When to see a doctor
If you feel like your heart is beating too fast or too slow, or it’s skipping a beat, make an appointment for a health checkup. You may be told to see a doctor trained in heart diseases, called a cardiologist.
Get emergency medical care if you have these heart symptoms:
- Chest pain.
- Shortness of breath.
- Fainting.
Always call 911 or your local emergency number if you think you might be having a heart attack.
A type of arrhythmia called ventricular fibrillation can cause a dramatic drop in blood pressure. This can cause the person to fall to the ground within seconds, also called collapse. Soon the person’s breathing and pulse will stop. Ventricular fibrillation is an emergency that needs immediate medical help. It’s the most frequent cause of sudden cardiac death.
If this happens, follow these steps:
- Call 911 or your local emergency number.
- If there’s no one nearby trained in cardiopulmonary resuscitation (CPR), provide hands-only CPR. Push hard and fast on the center of the chest. Do 100 to 120 compressions a minute until medical help arrives. You do not need to breathe into the person’s mouth.
- CPR helps keep blood flowing to the organs until an electrical shock can be given with an automated external defibrillator (AED). An AED is a device that delivers a shock to restart the heart.
- If an AED is available nearby, have someone get the device and follow the instructions. No training is required to use it. The device tells you what to do. It’s programmed to allow a shock only when appropriate.
Causes
To understand the cause of heart arrhythmias, it may help to know how the heart works.
How does the heart beat?
The typical heart has four chambers.
- The two upper chambers are called the atria.
- The two lower chambers are called the ventricles.
The heart’s electrical system controls the heartbeat. The heart’s electrical signals start in a group of cells at the top of the heart called the sinus node. They pass through a pathway between the upper and lower heart chambers called the atrioventricular (AV) node. The movement of the signals causes the heart to squeeze and pump blood.
In a healthy heart, this heart signaling process usually goes smoothly, resulting in a resting heart rate of 60 to 100 beats a minute.
But some things can change how electrical signals travel through the heart and cause arrhythmias. They include:
- A heart attack or scarring from a previous heart attack.
- Blocked arteries in the heart, called coronary artery disease.
- Changes to the heart’s structure, such as from cardiomyopathy.
- Diabetes.
- High blood pressure.
- Infection with COVID-19.
- Overactive or underactive thyroid gland.
- Sleep apnea.
- Some medicines, including those used to treat colds and allergies.
- Drinking too much alcohol or caffeine.
- Illegal drug use or drug misuse.
- Genetics.
- Smoking.
- Stress or anxiety.
Risk factors
Things that may increase the risk of heart arrhythmias include:
- Coronary artery disease, other heart problems and previous heart surgery. Narrowed heart arteries, a heart attack, heart valve disease, prior heart surgery, heart failure, cardiomyopathy and other heart damage are risk factors for almost any kind of arrhythmia.
- High blood pressure. This condition increases the risk of developing coronary artery disease. It also may cause the walls of the left lower heart chamber to become stiff and thick, which can change how electrical signals travel through the heart.
- Heart problems present at birth. Also called congenital heart defects, some of these problems may affect the heart rate and rhythm.
- Thyroid disease. Having an overactive or underactive thyroid gland can raise the risk of irregular heartbeats.
- Obstructive sleep apnea. This condition causes pauses in breathing during sleep. It can lead to a slow heartbeat and irregular heartbeats, including atrial fibrillation.
- Electrolyte imbalance. Substances in the blood called electrolytes help trigger and send electrical signals in the heart. Potassium, sodium, calcium and magnesium are examples of electrolytes. If the body’s electrolytes are too low or too high, it may interfere with heart signaling and lead to irregular heartbeats.
- Some medicines and supplements. Some prescription medicines and certain cough and cold treatments can cause arrhythmias.
- Excessive alcohol use. Drinking too much alcohol can affect electrical signaling in the heart. This can increase the chance of developing atrial fibrillation.
- Caffeine, nicotine or illegal drug use. Stimulants can cause the heart to beat faster and may lead to the development of more-serious arrhythmias. Illegal drugs, such as amphetamines and cocaine, may greatly affect the heart. Some may cause sudden death due to ventricular fibrillation.
Complications
Complications depend on the type of heart arrhythmia. Possible complications of heart arrhythmias include:
- Blood clots, which can lead to stroke.
- Heart failure.
- Sudden cardiac death.
Blood-thinning medicines can lower the risk of stroke related to atrial fibrillation and other heart arrhythmias. If you have a heart arrhythmia, ask a healthcare professional if you need to take a blood thinner.
If an arrhythmia is causing heart failure symptoms, treatment to control the heart rate may help the heart work better.
Prevention
Lifestyle changes used to manage heart disease may help prevent heart arrhythmias. Try these heart-healthy tips:
- Don’t smoke.
- Eat a diet that’s low in salt and saturated fat.
- Exercise at least 30 minutes a day on most days of the week.
- Maintain a healthy weight.
- Reduce and manage stress.
- Control high blood pressure, high cholesterol and diabetes.
- Get good sleep. Adults should aim for 7 to 9 hours daily.
- Limit or avoid caffeine and alcohol.
 MATCDHAKA – Medical Assistant Training Centre in Dhaka Pharmacy, Veterinary, Dental, Nursing, Pathology, Physiotherapy and Homeopathy Training Institute in Dhaka
MATCDHAKA – Medical Assistant Training Centre in Dhaka Pharmacy, Veterinary, Dental, Nursing, Pathology, Physiotherapy and Homeopathy Training Institute in Dhaka